If the COVID-19 pandemic grows rapidly in South Dakota — as it has in other states and nations — the state’s hospital systems are likely to be quickly overwhelmed, according to medical experts in South Dakota and elsewhere.
It is unknown if the state has enough ventilators or intensive-care beds, and patients in rural areas or smaller cities would likely need to be transported to urban areas to receive proper care for the disease, they say.
South Dakota’s public health and medical providers say they are confident in the health-care system’s ability to handle a surge in COVID-19 patients, but experts worry that if an outbreak grows too fast, hospitals will be unable to properly house and care for all patients.
Nationally, an analysis of hospital capacity by researchers at Harvard University found that even a moderate outbreak, in which 40% of adults contract the virus, could overwhelm hospitals all over the country.
Though specific numbers are difficult to come by, national statistics and survey data suggest that there simply is not enough room in intensive care units or enough mechanical ventilators in the country, let alone in South Dakota, to serve all the patients that would need help breathing if the spread of the COVID-19 virus cannot be controlled.
The number of hospital beds and ventilators available in South Dakota, and how many of those beds can be used for intensive care, isn’t publicly available, and state officials and medical providers refuse to release the data.
State public health officials have access to a database called HAv-BED that tracks hospital bed availability in near-real time. Department of Health spokesman Derrick Haskins told South Dakota News Watch that assigning a hard number to ICU and ventilator availability is difficult because the numbers change multiple times per day. The state also maintains a stockpile of medical supplies for emergencies that does include ventilators, but Haskins wouldn’t say how many ventilators were in the stockpile.
Two of the state’s major hospital systems, Avera Health and Sanford Health, also declined to disclose to News Watch how many ventilators they currently have available.
“The reality is, even though we have excellent health care here … there are still more residents in the upper Midwest than there are beds and ventilators,” said Dr. Jeremy Storm, an infectious disease specialist from Sioux Falls. “The numbers, I think, are pretty dramatic. There is, approximately, a 20% hospitalization rate, 20% of hospitalized patients requiring an ICU bed and approximately 50% of them are ending up on a ventilator.”

Scarcity of hospital beds and ventilators could mean that COVID-19 patients, particularly those in rural areas of South Dakota, would have to be transported between hospitals. Hospitals in Sioux Falls, for example, might take more COVID-19 patients who need help breathing, while the Sanford Hospital in Chamberlain might be asked to take patients who don’t need such intense treatment, said Dr. Mike Wilde, vice president of Sanford Health in Sioux Falls.
“It appears this illness does cause a dependence on advanced life support and a lot of that support really can only be found at a larger facility,” Wilde said. “But we still need to take care of our patients that come in with illnesses that we commonly see. Perhaps some of our network partners could have some of those patients go to their facilities while, in turn, we take the patients with the needs specific to (COVID-19).”
The American Hospital Association, which annually surveys about 80% of U.S. hospitals on bed and equipment availability, estimates there are about 924,000 fully staffed hospital beds in the country, if federal facilities are included in the count. Community hospitals account for a little more than 790,000 beds in a country of 328 million people, according to AHA data.
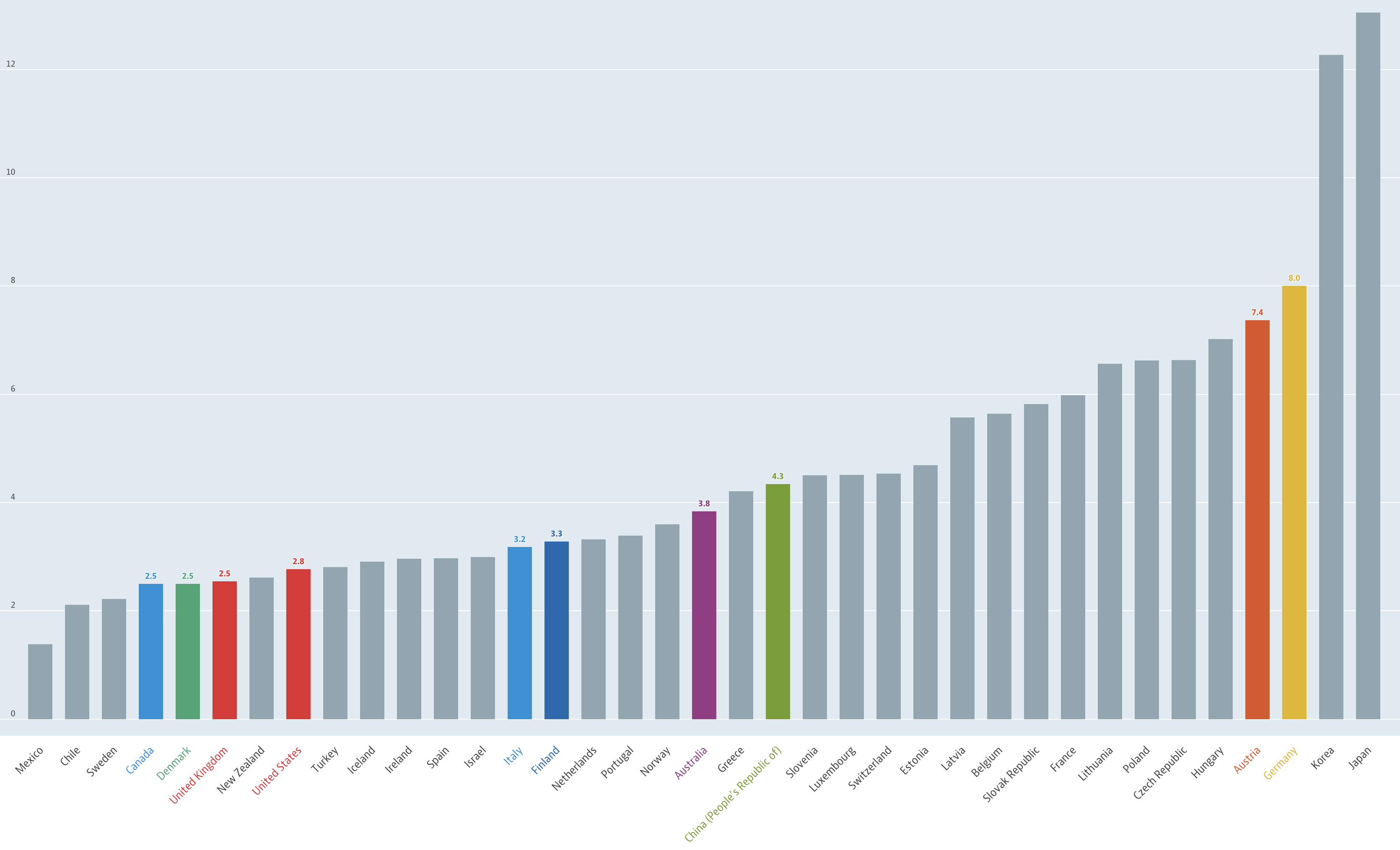
The U.S. also has a relatively low ratio of hospital beds in relation to population when compared to other industrialized countries. The International Organization for Economic Cooperation and Development estimates the U.S. has about 2.8 hospital beds per 1,000 people. Meanwhile Italy, a country that has seen hospitals overwhelmed by a massive, fast-moving COVID-19 outbreak, has roughly 3.2 beds per 1,000 people, according to OECD data. China, where the COVID-19 virus originated, is estimated to have 4.3 beds per 1,000 people; Japan has the most at more than 12 per 1,000 people.
Another choke point, experts say, will be the availability of intensive care units and mechanical ventilation equipment. As many as 20% of people hospitalized for COVID-19 need intensive care. About half of COVID-19 patients in the ICU need help breathing because the virus causes pneumonia, which impedes the ability of a person’s lungs to absorb oxygen.
Exactly how many ventilators U.S. hospitals have is not known. The most recent data on the subject is more than 10 years old, according to the Society of Critical Care, an association of intensive care professionals. The data suggests there were around 62,000 ventilators that can help children and adults available in the U.S. in 2009. Another roughly 36,700 older model ventilators were available for use on adults, an SCC report said.

"The reality is, even though we have excellent health care here … there are still more residents in the upper Midwest than there are beds and ventilators ... the numbers, I think, are pretty dramatic." -- Dr. Jeremy Storm, an infectious disease specialist based in Sioux Falls
Storm said countries such as Italy and Iran, where COVID-19 has run rampant, offer cautionary tales for South Dakota. In Italy, more than 27,900 people have been diagnosed with COVID-19 and more than 2,500 people have died, according to the World Health Organization. Hospitals there have been overwhelmed and doctors have been forced to prioritize which patients can get life-saving care and which are left to face illness and possibly death without treatment.
In the U.S., President Donald Trump on March 17 suggested that federal officials and the military could build temporary medical facilities to handle an influx of new COVID-19 patients, if needed. The announcement came as the number of confirmed COVID-19 cases nationwide topped 8,500 and the number of reported deaths from the disease rose to 140.
As of March 18 in South Dakota, 11 people are confirmed to have contracted COVID-19 and one man has died. A total of five confirmed cases have been found in Minnehaha County, the state’s most populous county. The rest of the confirmed cases have been spread across six counties in the eastern half of the state. One man from Pennington County — who became the state’s only confirmed fatality due to COVID-19 — was found to have the disease but had been outside the county for more than two weeks when he died.
Each confirmed case of COVID-19 in South Dakota is thought to have originated from outside the state, officials say. That is good news for South Dakota hospitals because it suggests community-level transmission hasn’t started yet. However, it is likely that there are many more people infected with COVID-19 than have been tested for the disease.
“There is a limiting factor right now, which is a number of tests that can be performed. So, there’s more cases out there than we’ve even identified,” Storm said.
State Epidemiologist Joshua Clayton announced on March 18 that the state health lab had run out of testing supplies on March 16 and wasn’t able to run more tests. The difficulties in completing tests for COVID-19 are a big reason why the Centers for Disease Control and Prevention and medical professionals have been pleading with all South Dakota residents, whether sick or not, to distance themselves from others and wash their hands regularly.
South Dakota hospitals have been working with first-responders to plan strategies for dealing with mass casualty events, mass radiation exposure and even global pandemics for more than a decade. Five years ago, the state’s hospitals spent a year planning and training to deal with a coronavirus epidemic, said Lynn DeYoung, executive director of the South Dakota Healthcare Coalition. The organization serves as a coordinator for medical disaster planning and training.
New innovations such as telemedicine also will play a critical role in helping keep doctors and nurses from being infected with COVID-19 and in dealing with long-term shortages of health-care workers. The federal Centers for Medicare and Medicaid Services on March 17 expanded its coverage of telehealth services to include in-home, virtual doctor visits for routine checkups.
“We’re pretty blessed that this has come to us at this point, rather than, say, about 15 years ago,” said Dr. David Basel, vice president of clinical quality at Avera Medical Group. “We’ve had time to prepare for this, develop a lot of these lines of communication between the CDC, the state Department of Health, other hospitals and other community resources and so that’s really helped prepare us to handle this new, novel threat.”
Flexibility within the health-care community will be critical to helping manage an influx of COVID-19 patients if they arrive, providers said.
“Even in times where there is not a crisis or emergency, we are continuously disaster planning and high-surge planning for situations like this,” said Wilde. “The question does keep coming up regarding bed numbers. The reality is, we can really move that number around based on need in the moment, on a day-to-day basis. We have a physical number of ICU beds, but that can move very quickly.”
In terms of hospital bed availability, South Dakota is in decent shape compared to the rest of the country. The state has more hospital beds per person, around 4.8 beds per 1,000 people, than any other state, according to an analysis by the Kaiser Family Foundation, a nonprofit that studies the health-care industry.
Gov. Kristi Noem held a meeting and press conference Wednesday with officials from Monument Health, formerly Regional Health, that provides health care to much of western South Dakota, including Rapid City. Monument CEO Paulette Davidson said at the press conference that the medical group has undergone extensive preparations to handle the COVID-19 epidemic.
“We have spent the last several weeks and actually months across the western South Dakota region preparing for COVID-19,” Davidson said. “We brought our clinical teams together, our physicians and our caregivers, our leaders, to prepare for what could happen in western South Dakota and we are well prepared. We have a large health system in our community and our region, we have providers outside Monument Health, we have clinicians that are all doing what needs to be done to take care of our communities.”
Noem said at the press conference that she has spoken with health and government officials from other states and in Washington, D.C. and is confident South Dakota is taking appropriate steps to slow the spread of the virus.
“The focus we have is on management,” Noem said. “It’s on making sure that going forward that we’re taking actions to avoid overwhelming our healthcare systems.”
Noem said she has met with leaders from Sanford and Monument health systems, and that “they’re very comfortable with where we are as a medical community and our response.”




