Editor’s note: This article was produced through a partnership between South Dakota News Watch and the Solutions Journalism Network, a national non-profit group that supports rigorous journalism about responses to problems.
PIERRE, S.D. – Public health experts are questioning the extent and effectiveness of contact-tracing efforts in South Dakota and across the country, arguing that an inadequate number of investigators and lags in testing times have reduced the efficacy of the tracing process.
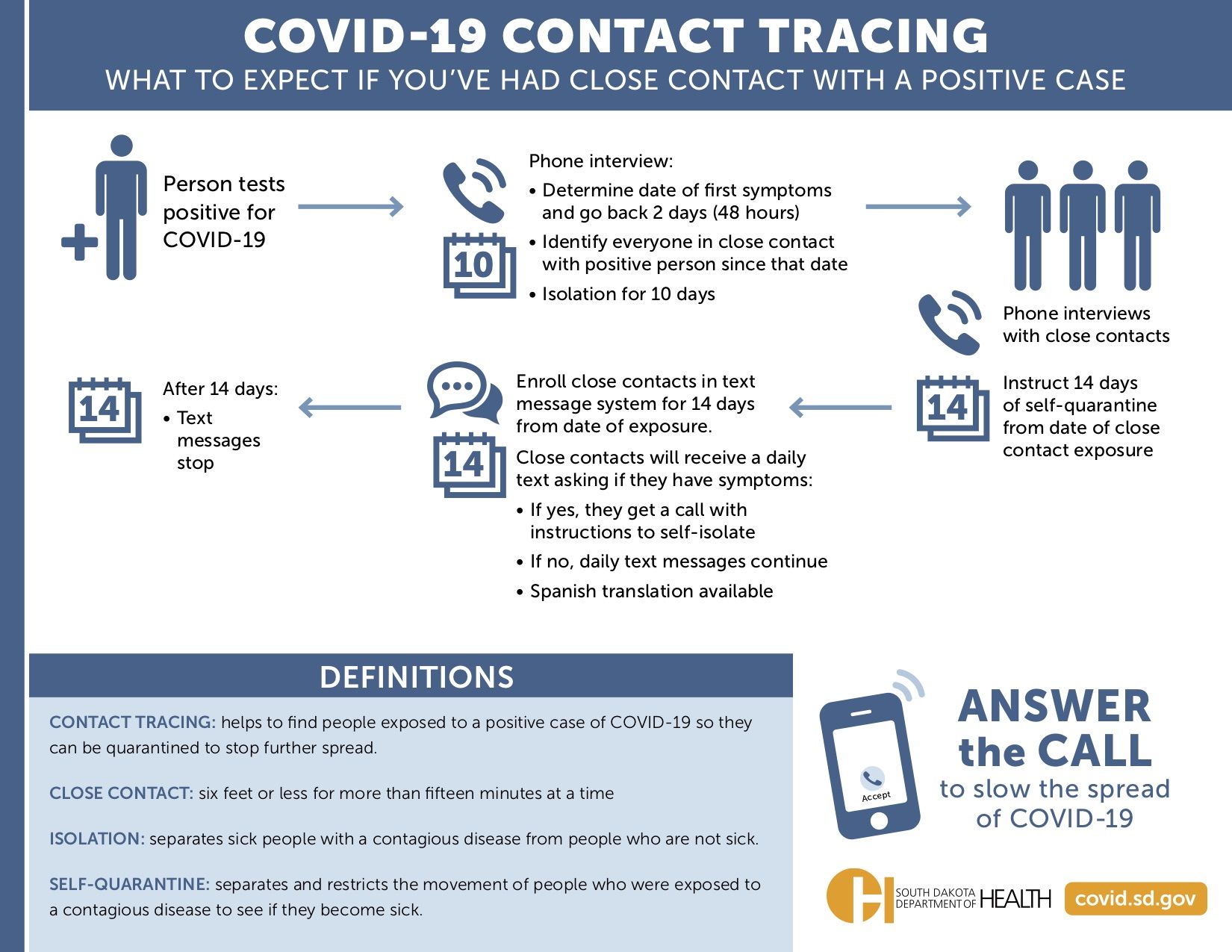
Contact tracing aims to reduce the spread of infectious diseases, including COVID-19, by quickly identifying people who may have been exposed to the virus. Investigators question people who test positive for the virus and then try to determine who else they may have come in contact with. Those people are then warned to isolate, watch for symptoms and get tested if they feel sick.
The process is seen as a critical tool in the fight against COVID-19 and other diseases such as tuberculosis because it can break or slow the cycle of transmission from one person to another.
When combined with high rates of testing and social distancing, contact tracing has been shown to slow the spread of COVID-19 and speed up the ability of countries such as South Korea, Singapore and Germany to safely re-open their national economies.
Investigating COVID-19 cases has taken on heightened importance in South Dakota in recent weeks as the state has seen a surge in its number of new cases. On Aug. 20, South Dakota reported 125 new cases of the disease and had the nation’s second-highest rate of transmission, according to state and federal data.
The state also reported on Aug. 20 that at least two dozen COVID-19 cases were related to the Sturgis motorcycle rally, including two notices about the potential for significant public exposures, and school districts and colleges were already reporting cases among students just days into the new academic year.
South Dakota Department of Health leaders say their contact-tracing efforts are keeping up with the increasing caseload. The state’s goal is to make contact with everyone who tests positive for COVID-19 in South Dakota within 24 hours of the department being notified of the new case.
The 131 contact tracers now working for the health department are making initial contacts with known COVID-19 patients within about 15 hours on average, said Cassie Deffenbaugh, who leads the contact-tracing team. The state contact-tracing workforce has grown to five times its pre-pandemic size since March, and has been able to identify 35,000 close contacts of coronavirus patients during the pandemic so far. Deffenbaugh said she is confident that the state’s contact tracers would be able to keep up with the virus.
“We are adequately staffed to be able to support our current workload,” Deffenbaugh said. “We are constantly assessing to make sure we are adequately staffed at this time and that we will be moving forward.”
But some disease researchers say the contact-tracing workforce is not widespread enough in South Dakota to handle the rising number of cases. Without increased availability of COVID-19 testing and speedier test result reporting — along with extensive social-distancing and increased mask usage — experts worry that contact tracers likely will be overwhelmed and the benefits of the process will be muted.
“I don’t think that we can afford, at this point, for contact investigation to stop the epidemic alone. It would have to be done at such a national scale with such speed and efficiency, that I don’t think that’s feasible,” said Travis Porco, an ophthalmological biostatistician and disease transmission researcher at the University of California at San Francisco who has been studying contact tracing since the pandemic began. “We really just don’t have a single magic bullet at this point, we need a little bit of everything to try to turn the tide.”

“[Contact tracing] is great because it can be a tool for protecting vulnerable people, we can find a lot of asymptomatic carriers and get them out of disease circulation. It's a big help, but it's not going to reduce the need, unfortunately, for masks and social distancing.” -- Travis Porco, University of California
The Centers for Disease Control and Prevention told Congress, in June, that the country needed a minimum of 100,000 contact tracers to adequately manage the COVID-19 pandemic.
But an Aug. 7 survey of state health departments conducted by Johns Hopkins Center for Health Security and National Public Radio found that there were just 41,122 contact tracers actively working in the U.S. Adding 59,000 more contact tracers to the workforce would cost billions of dollars, CDC officials said.
The Johns Hopkins/NPR survey also found that just three states — Maine, New Hampshire and Vermont — had enough contact tracers on staff to adequately track their COVID-19 cases. Three additional states — Montana, Michigan and Hawaii — would have enough contract tracers if they would bring in reserve staff. The South Dakota health department did not participate in the survey.
A News Watch analysis of the Contact Tracing Workforce Estimator created by the Fitzhugh Mullan Institute for Health Workforce Equity at George Washington University shows the state would need 638 contact tracers in order to adequately cover the average number of new cases found between Aug. 4 and Aug. 18. Hiring several hundred more contact tracers could cost millions of dollars and could likely take months.
Contact tracing can be an essential public health tool for managing a pandemic, according to the Centers for Disease Control and Prevention. Aggressively tracking down and identifying who, how and when people become infected with COVID-19 and then selectively quarantining people who have been in contact with or have been diagnosed with the virus can break chains of transmission. Breaking the chain of transmission can prevent widespread outbreaks, reducing both the number of deaths from the disease and its negative economic effects.
“Contact tracing is useful because it allows us to help people at direct risk of infection, rather than only being able to act in ways that help the whole community, which helps us use broad actions like shelter-in-place more sparingly, and also ensures that we can direct our time and attention to where they’re needed most.,” said Eric Lofgren, an epidemiologist and assistant professor at Washington State University.
South Korea, for example, was once second only to China in the severity of its COVID-19 problem. But an aggressive, nationwide contact-tracing campaign, combined with high levels of testing, have helped contain outbreaks and keep the number of new cases under control. Since the beginning of July, the country of 50 million has seen an average of fewer than 60 new cases per day.
In one well publicized incident, South Korea’s investigators identified a popular nightclub in the country’s capital, Seoul, as the source of a potential COVID-19 outbreak after someone at the nightclub tested positive for the virus. Contact tracers used surveillance cameras, credit card records and personal interviews to track transmission from the nightclub to a student, a taxi driver and someone who worked at a warehouse with 4,000 employees, all before they could spread the disease further. The outbreak was capped at 156 cases.
The South Korean economy, meanwhile, has remained largely open, though heavily impacted by declines in export trade due to the pandemic. South Koreans are still going to restaurants and bars and using air travel for vacations.
Contact tracing can also help identify people at the most risk from COVID-19 due to old age or a preexisting health condition such as diabetes early so they can be monitored more closely and provided health care more quickly when needed. Contact tracing is also about the only way to find people who are carrying the virus but aren’t displaying symptoms so they can be quarantined, Porco said. Any delay in testing people or in getting test results will reduce the value of contact tracing because infected people have more time to spread the illness to more people.
“What contact tracing gives you, if it’s done well, is the chance to out run the epidemic a little bit,” Porco said. “If you find a case fast enough. And you can find their contacts, you could intervene.”
Investigating disease transmissions through contact tracing is not a new concept in South Dakota. It has been common practice in the public health field for decades as an effective tool for helping to control the spread of infectious diseases such as tuberculosis or measles and even sexually transmitted infections such as syphilis or HIV.
Prior to the pandemic, the SDDOH employed 21 contact tracers officially known as Disease Intervention Specialists. After the pandemic began, the health department spent an additional $1.2 million on contact tracing and added 110 contact tracers, known as COVID Intervention Specialists. They are spread out among health department offices in Aberdeen, Pierre, Rapid City, Sioux Falls and Watertown. Increased funding for contact tracing came as part of federal pandemic relief efforts such as the CARES Act.
Every person who tests positive for SARS-COV-II, the virus that causes COVID-19, is supposed to be investigated by the state’s contact-tracing team, Deffenbaugh said. The contact tracing process begins when DOH is notified that someone has tested positive for the virus. South Dakota state law requires healthcare providers to notify the state immediately when they suspect someone has a respiratory illness such as COVID-19.
The state’s goal is to make contact with a person who has tested positive for the COVID-19 virus within 24 hours of the department being notified of the test. The initial contact includes some education on COVID-19 and what to expect from the disease as well as how to avoid spreading the disease to others.
Contact tracers can even help people find places to self isolate if quarantining in their home isn’t feasible, Deffenbaugh said. So far, the health department has helped 48 people find a place to quarantine outside their home.
But the most important thing contact tracers do is identify a COVID-19 patient’s close contacts, which includes anyone the patient had been within six feet for 15 minutes or more up to 48 hours before showing symptoms. The interview includes questions about the patient’s workplace, social gatherings, activities and home life.
The idea is to collect as much contact information on a patient’s close contacts as possible and then notify each close contact to alert them of the possible exposure. The patient’s close contacts are then advised to self isolate, monitor themselves for symptoms and get tested for the disease if symptomatic.
“Ultimately, our goal is to do everything that we can to help them identify the people that may have been exposed,” Deffenbaugh said. “People are very good at working with us and ultimately they care about the people that they may have exposed.”

Once the investigation has been completed, each contact is supposed to be enrolled in a daily monitoring program so contact tracers can follow-up via text message or phone calls to ask about symptoms and provide resources for quarantining or isolating. Monitoring lasts until a person is deemed recovered from COVID-19 or fails to develop symptoms for up to 14 days after being exposed.
Sometimes a contact-tracing investigation reveals that someone spent time at a crowded event or a bar and can’t provide information on everyone they came into close contact with, Deffenbaugh said. When that happens, the state issues an alert with the date, time and location of the potential exposure. Recent examples include notices issued on Aug. 18 and 20 after a person who spent time in a Sturgis saloon and a tattoo parlor worker tested positive for COVID-19. On Aug. 14, the state issued an alert after a person who attended a concert at the Sioux Empire Fairgrounds in Sioux Falls tested positive for the virus.
Contact tracing is an expensive, resource-intensive process. It requires many people making many contacts by phone and aggressively investigating every new COVID-19 case thoroughly and quickly. Testing for the virus must be conducted quickly and results from tests must be turned over to health departments in a timely fashion. Tests for the virus also need to be widely available to anyone, not just those displaying symptoms, Porco said.
“Contact investigation, if done well, is very intensive. It takes a lot of resources,” Porco said.
For all of its importance, contact tracing has a number of shortfalls. For one thing, contact tracing in South Dakota relies on people to answer phone calls, often from strange numbers. In today’s world of random robo-calls and phone scammers, that can be a big ask, Deffenbaugh said.
“We do have instances where we may not be able to get a hold of someone; that is one of the challenges we have,” Deffenbaugh said. “Obviously there are a lot of unknowns, [but] as we’re doing our case investigations, we are identifying those contacts.”
Because contact tracing is such an expensive, time-consuming activity, public health agencies can struggle to scale up their efforts when disease transmission rates are high. Transmission rates and case numbers are high enough now, Porco said, that there is likely no way to bring enough new contact tracers online fast enough to slow the spread of the virus.
Some areas should consider another lock down, Porco said, and testing availability as well as the speed of testing need to be improved. The use of masks and social distancing could be improved, he said.
“[Contact tracing] is great because it can be a tool for protecting vulnerable people, we can find a lot of asymptomatic carriers and get them out of disease circulation,” Porco said. “It’s a big help. But it’s not going to reduce the need, unfortunately, for masks and social distancing.”





